What is a Fungal Nail Infection?
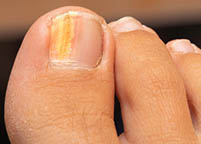
Fungal nail infections, or Onychomycosis, are very common. They usually affect adults, men more so than women, and they are more common as you get older.
Causes:
- It is a secondary infection caused by Athlete’s Foot (Tinea Pedis) on the skin.
- It can spread from the skin to the nails if the nail is damaged, so treating Athlete’s Foot with an anti-fungal cream as soon as possible is important.
- Trauma to the nail allows the fungus to spread. This can be something as simple as wearing tightly-fitting shoes regularly
- You are at a higher risk if in poor health as your immune system will be low
- You are more prone if you have sweaty feet and wear dark socks, perfect conditions for fungal infections
Symptoms:
- It usually starts with just one nail
- The skin around the nail may be red and inflamed
- Nail may appear thickened, yellowish/brown or green/black colour, brittle,
- Eventually the nail becomes soft and crumbles, it may come away from nailbed
- Nail and nailbed can be destroyed permanently if not treated
- It can lead to ingrowing toenails and/or infection if left untreated
- It may spread to other nails if they too become damaged and open to infection
Treatments:
Fungal nail infections are difficult to treat as the nail acts as a barrier to the nailbed. This is where the infection is worse, and, therefore, means most ‘home treatments’ are ineffective. It is important to seek professional help to increase your chances of success.
A Podiatrist or Foot Health Practitioner will take a medical history, examine your feet thoroughly, including the skin for any signs of Athlete’s Foot. They will then discuss the various treatments available:-
- Amorolfine 5% Nail Lacquer – this can be bought over-the-counter from your pharmacist. It can penetrate the nail plate unlike many other fungal nail treatments available to buy, so it is more effective. It is applied once a week over a long period of time. The nail must be filed to help the treatment penetrate so we would recommend you visit a professional to thin it for you.
- Lamisil 1% Spray – this is effective if the nailbed is exposed, so the nail must be cut back or drilled.
- Oral medication – Terbinafine. These tablets must be prescribed by your G.P. The G.P. will not prescribe them unless a nail sample has come back positive for Onychomycosis. You will need to have regular blood tests to check liver function. They can only be taken for a few months. Topical treatments can be used in conjunction with these.
- Clearanail Treatment– a Podiatrist can use a computerized drill to painlessly drill holes in the nail and apply terbinafine directly to the nailbed. It usually requires up to 3 treatments. This is a relatively new treatment, but early indications are good.
- Cold Laser Treatment – some Podiatrists favour a low-level laser treatment, such as Lunula laser Treatment, which is also painless as it is non-thermal unlike previous laser treatments.
N.B. Unfortunately, no fungal nail treatment currently on offer can guarantee complete success and, in many cases, the fungal nail infection can return.
How do you know the nail has improved?
The fungi that are killed remain in the nail until it has grown out so it will still be visible. New, healthy nail appears from the nailbed. This will take many months, even one-to-two years, depending on nail-growth!
Prevention:
- Dry feet thoroughly after baths/showers
- Treat Athlete’s Foot immediately
- Change socks daily
- If you suffer from fungal infections, disinfect your footwear regularly
- Avoid injury to the nails. This includes pressure and friction from footwear
- Do not use ordinary nail polish which are damaging to nails and encourage infection. Instead, use Podiatrist-approved Dr.’s Remedy Nail Care. (Available online or in clinic)
- Avoid pedicures if you have concerns about hygiene levels or are not sure whether the instruments used are sterilised
Not all the current treatments are available without seeking the help of a professional, whether that be your G.P., Podiatrist or Foot Health Practitioner. They will advise you and direct you, so you can make an informed decision on what treatment will suit, based on your health and lifestyle.
(This article is based on recent guidelines issued by The SMAE Institute and on Dermatology lectures attended at the Southern Chiropody, Podiatry and FHP Association, as well as my personal experience in my clinic)